Photo credit: Getty Images
Understanding an important billing notification for patients.
By Mark K. Davis, OD
Jan. 10, 2024
You probably have heard of an Advance Beneficiary Notice (ABN), but may not be clear on exactly what it is or what you, as a provider, need to be aware of as you bill for your services. Here are the most important points to keep in mind about ABNs.
What is It?
An advance written notice of non-coverage helps Medicare Fee-for-Service (FFS) patients choose items and services Medicare usually covers, but may not pay because they’re not medically necessary or considered experimental (think Category 3 CPT codes – temporary, ending in the letter T). You communicate these financial liabilities and appeal rights and protections through notices you give your patients. If you don’t provide your patients with the required written notices, Medicare may hold you financially liable if they deny payment (in other words, you cannot balance bill the patient).
Other Articles to Explore
There are three types of ABNs. There is one for providers (both A & B), one for skilled nursing facilities and one for hospitals. We are interested in the provider designation. Under the provider designation, there are two choices:
- Part B (outpatient) items and services provided in offices, independent labs, skilled
nursing facilities (SNFs) and home health agencies (HHAs).
- Part A (inpatient) items and services provided by hospice providers, HHAs and religious
non-medical healthcare institutions (RNHCIs).
To transfer financial liability to the patient, you must issue an advance written notice of non-coverage. You do this when a Medicare item or service isn’t reasonable or necessary under program standards, including care that’s:
- Not indicated for the diagnosis, treatment of illness, injury, or to improve the functioning of a malformed body member (you can’t take retinal photos of diabetic patients that show no diabetic retinopathy and bill Medicare).
- Experimental and investigational or considered research only (again think of the Category 3 CPT codes that end in T. Some ophthalmic companies were pushing their VEP and ERG instruments for detecting glaucoma. This was voided by CMS as having no scientific justification).
- More than the number of services allowed in a specific period for that diagnosis (OCT for glaucoma patients is generally twice a year. Any more services than that and the patient may be required to pay for it or you write it off).
- Before providing a preventive service Medicare usually covers, but won’t cover in specific situations when services exceed frequency limits (Medicare covers one annual eye exam to test for diabetic retinopathy among diabetics, even if no retinopathy is found. Remember, no photos, if no retinopathy)
Events Prompting an Advance Written Notice of Non-Coverage
Initiations:
- Initiations happen at the beginning of a new patient encounter, start of a plan of care (POC), or when treatment begins. If you believe at initiation Medicare won’t cover certain items or services because they’re not reasonable and necessary, you must issue the notice before the patient gets the non-covered care to transfer financial liability.
Reductions:
- Reductions happen when a component of care decreases (for example, frequency or service duration). Don’t issue the notice every time there’s a care reduction. If a reduction happens and the patient wants to continue getting care no longer considered medically reasonable or necessary, you must issue the notice before the patient gets the non-covered care to transfer financial liability.
Terminations:
- Terminations stop all or certain items or services. If you terminate services and the patient wants to continue getting care no longer considered medically reasonable or necessary, you must issue the notice before the patient gets the non-covered care to transfer financial liability.
An ABN remains effective after delivery if there’s no change in:
- Care described on the original ABN
- Patient’s health status
- Medicare coverage guidelines for the items or services in question (for example, updates or changes to the policy of an item or service)
Note: If any information featured in the above bullets change during treatment, issue a new ABN
An advance written notice of non-coverage should be:
- Issued (preferably in person) and understood by the patient or their representative.
- Completed on the approved, standardized notice format (when applicable), with all required blanks completed. It can’t exceed one page. You may include attachments listing additional items and services. If you use attachment sheets, they must clearly match the items or services in question with the reason a denial is expected and cost estimate information. The patient should be able to read it. Medicare permits limited advance written notice of non-coverage customization, such as pre-printing information in certain blanks.
- Issued far enough in advance for potentially non-covered items or services, so the patient can consider available options.
- Explained in its entirety, with you answering all notice-related questions.
- Signed and dated by the patient or their representative after they select an option. If you issue the notice electronically, offer the patient a paper copy and keep a copy for your records (whether signed on paper or electronically). If you maintain electronic medical records, you may scan the signed hard copy.
- Kept for five years from the date-of-care delivery when no other requirements under state law apply. You are required to keep all notice records, including when the patient declined care, refused an option or refused to sign the notice.
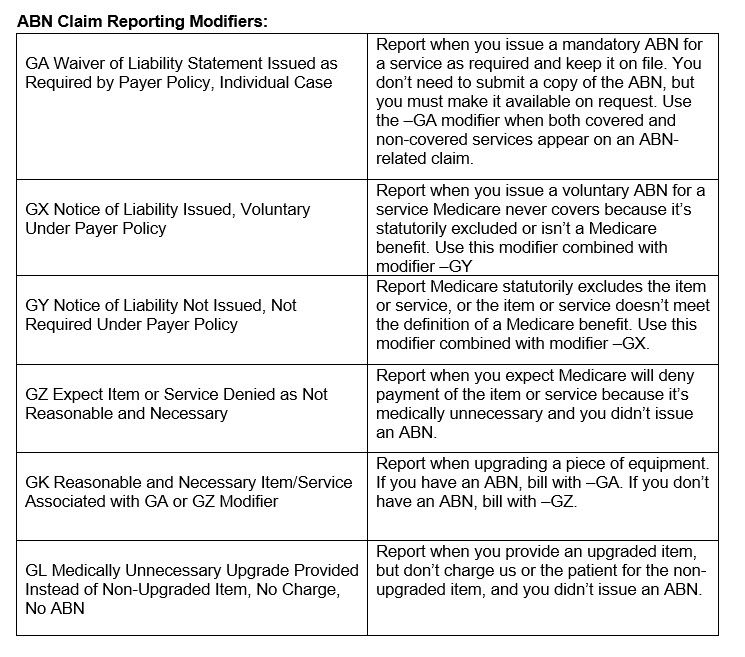
See below for the official ABN form provided by Medicare. For further in depth explanation of the ABN, Click HERE.
Until next time; Happy Coding!

 Mark K. Davis, OD, is a Therapeutic Optometrist and Optometric Glaucoma Specialist, Diplomate, American Board of Optometry, Adjunct Assistant Professor, University of Houston College of Optometry and Chief of Optometry, 147th Medical Group. He is Lt Col, Texas Air National Guard, Ellington Field JRB, Houston, Texas. To contact him: mkdavisod@gmail.com
Mark K. Davis, OD, is a Therapeutic Optometrist and Optometric Glaucoma Specialist, Diplomate, American Board of Optometry, Adjunct Assistant Professor, University of Houston College of Optometry and Chief of Optometry, 147th Medical Group. He is Lt Col, Texas Air National Guard, Ellington Field JRB, Houston, Texas. To contact him: mkdavisod@gmail.com