By Peter J. Cass, OD
July 27, 2016
Dry eye is affecting anincreasing number of people. Your practice can capture the full potential of treating these patients with dry eye, using technology that helps the OD to diagnose and treat this condition effectively.
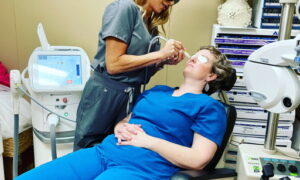
My practice has invested in LipiFlow, an electronic device cleared by the U.S. Food and Drug Administration (FDA) for treatment of meibomian gland dysfunction. It uses an applicator which heats and then applies pressure to the Meibomian glands from both sides of the lid. The applicator rests on a shield that fits over the cornea (much like a scleral lens) and protects the cornea during the treatment process.
The LipiView device is an imaging and digital video device that allows imaging of the Meibomian glands, imaging of blockage in the glands, lipid layer thickness measurement, blink rate measurement and lid closure.
The LipiView guides the treatment protocol. Patients who have gland atrophy, or gland blockage, benefit from the procedure. Patients with severe gland dropout, or with minimal blockage, benefit the least, while patients with minimal gland dropout and severe blockage benefit the most.
The LipiFlow procedure is not covered by insurance, so it is an out-of-pocket expense for the patient. We do not charge for the LipiView, and fees vary by region for the LipiFlow, with $1,400 being an average in my region (Texas). Surprisingly, there is little resistance to the price from patients, and I really enjoy the private-pay model.
Many insurance providers are racing each other to the bottom of reimbursement rates to providers, so whenever we can take insurance out of the equation is a positive step. Because the out-of-pocket expense is high, not all patients can afford the procedure, so traditional treatment options are offered to them. While those treatment options are not as effective, they still offer some therapeutic benefit.
We have only had the device for three months, but it has been profitable from the first month. We are doing about one procedure per week. The device is breakeven at two procedures, and profitable at three procedures per month. Using our screening protocol we have been scheduling about one full dry eye exam workup per day. We have set a goal of 10 per month, and should be able to achieve that within just a few months.
The equipment has a very small footprint. The LipiView is about the size of an auto-refactor, and sits on our pre-test table with our auto-refractor. The LipiView is networked wirelessly, and images and videos can be viewed from any workstation in any exam lane. The LipiFlow takes up even less space (about as much as a computer monitor) and is lightweight and portable and can be moved from room to room.
Invest in Advanced Care
We added the LipiFlow device into my practice because of the leap forward in dry eye disease care that it represents. Evaporative dry eye (due to Meibomian gland disease) is the cause in over 80 percent of the estimated 23 million dry eye sufferers in the U.S. Traditional therapies, such hot compresses and lid massage, are the right approach to the treatment of evaporative dry eye disease, but they are unfortunately minimally effective. Hot compresses because fat and muscle anterior to the Meibomian glands dissipate heat applied to the surface. Lid massage because pressure applied from one side of the lid is reduced by posterior displacement of the lid against the globe. The LipiFlow device is much more effective because it can apply heat and pressure to both sides of the lids.
The LipiView allows me to objectively measure and quantify gland dropout, gland blockage, lipid layer thickness, blink rate, partial blinks and lid closure. Since the measurements are objective and repeatable they have been extremely useful in making a diagnosis, establishing a more effective treatment protocol, and objectively monitoring progress of treatment. Additionally, the images and results can be shared with the patient for educational purposes. Having used the LipiView for some time now, I have been surprised at how much more informed my diagnosis and management decisions are, and find it comparable to using an OCT to diagnosis and manage glaucoma.
Enhance Patient Experience
LipiView and LipiFlow have definitely changed the way I diagnose and manage dry eye. I would not want to treat dry eye now without these instruments, and I am excited about the changes it has made to the practice and my evaluation and management of dry eye disease. LipiFlow adds a spa-like experience to the office and has been received really well by our patients. I have been surprised at how quickly patients accept the procedure and how excited about it they are. It has provided a huge internal marketing boost for our practice, and helps us to differentiate ourselves. It’s a way to combat the negative effects and trends in third-party payment. LipiFlow does not replace other treatments for dry eye, rather it compliments much of what we already do for dry eye: Eye drops, prescription medications, punctal plugs, eye lid scrubs, warm/hot compresses and Omega – 3 Oils.
Project ROI
Depending on the price charged for the procedure, the total cost of the systems should be recouped in about 60 procedures (at a $1,500 bilateral charge) to 90 procedures (at a $990 bilateral charge). These calculations take into account the cost of consumable supplies that are used during the procedure. We purchased the system through a lease-to-own program with Stearns bank.
The combined cost of the LipiFlow and LipiView is in the high $60,000 dollar range. From a practice management standpoint, providers considering purchasing any instrument should always calculate the potential return on investment. If an instrument is beneficial for patient care, and a provider can expect to collect twice the note in a given month, the instrument is usually a good purchase for the practice.
The applicators for the LipiFlow instrument are disposable and cost about $175, for a total cost of about $350 per procedures.
Break-even on LipiFlow is 60-90 procedures depending on the price the practice charges for the procedure.
However, the device can be profitable from the first month. In fact, based on my monthly note, and the amount our office charges for the procedure, we make money with as few as three procedures per month (and we have been profitable from the first month we purchased the device).
Screen All Patients
We screen everyone with the LipiView (using an abbreviated imaging protocol) and show the images to the patient when we notice gland dropout or blockage. Those patients are then scheduled for a full dry eye workup and a full LipiView exam is performed at that dry eye exam. The images and videos produced by the LipiView system are essential to explain to the patient why the LipiFlow procedure is worth the expense.
I show the images to the patient, and go through the tests one-by-one with each patient. We have quick reference cards we hand to the patient and ask them to match the severity on the card to the images they see on the screen. Patients are very good at assessing their own level of Meibomian gland disease, and making them part of the process helps them to accept recommendations for care. The findings on the LipiView usually very accurately predict findings on slit lamp examination (e.g. severe blockage predicts poor expression, thin lipid layer predicts low TBUT, etc.). Our dry eye workup includes:
OSDI risk factors for dry eye (done by technician)
SPEED test for symptoms, frequency, and severity of dry eye (done by technician)
LipiView gland dropout imaging (done by technician)
LipiView gland blockage imaging (done by technician)
Lipid layer thickness measurement (done by technician)
Blink rate measurement, including partial blink rate measurement (done by technician)
InflammaDry rapid, in-office MMP-9 tear analysis testing (done by technician)
Gland expression
Tear breakup time
Corneal and conjunctival staining
Re-treatment depends on the severity of the disease and patient involvement in self-care. Re-treatment is rarely needed sooner than six months, and many patients can go much longer if they are consistent with at-home maintenance. I often tell patients the LipiView can identify blockage in the glands in much the same way as x-rays can identify cavities. The LipiFlow can clear blockage in much the same way a dentist can repair a cavity. At-home hot compresses, lid massage and lid scrubs can prevent the need for re-treatment in much the same way that flossing, brushing and rinsing can prevent cavities. I really like the dental analogy because of the acceptance that patients have of frequent dental exams and out-of-pocket expenses for dental care.
Train to Use Instrumentation
The LipiView and LipiFlow are very easy to use.
As with any imaging device, staff can usually get the basics down with a couple hours of training, but good quality images with the LipiView take practice and get better quickly. My staff was consistently producing high quality images within a week. The Lipiflow was surprising easy for my staff to learn. It is similar to inserting a scleral lens. My assistant was a little nervous with the first couple patients, but quickly became very competent with the device and applicators.
The vendor provided complimentary training (as most do at that price point) and has been extremely engaged in ongoing training, coming once or more per week for several weeks. The vendors worked with my staff on setup, training and staff-patient scripting. They also worked with me on interpretation and patient communication. They were present on our first treatment day (which was actually a very fun day). The business model for TearScience, the company that manufactures the LipiView and LipiFlow instruments, includes revenue from sales of applicators, and reps are evaluated on sales of applicators. This business model incentivizes reps to make regular visits to the office to make sure that everything is going well, and to make sure that the staff is well trained.
Refine Dry Eye Protocol
My office is very busy, and I personally see 40-50 patients per day, so efficiency is very important to us. TearScience’s normal protocol did not work well for us, but the rep was quick to work with us to modify the protocol to fit the way our office functions. Making minor tweaks to the protocol allowed us to incorporate the equipment, testing and procedures into our office flow without slowing us down.
Promote Instrumentation
We mainly promote through our Facebook page and internal marketing. For internal marketing, once we identify a patient with dry eye signs or symptoms, we discuss the findings with them and provide them with a dry eye info sheet, and a LipiFlow brochure.
Peter J. Cass, OD, is the owner of Beaumont Family Eye Care in Beaumont, Texas. To contact: pcassod@gmail.com