By Aaron Neufeld, OD
Oct. 26, 2016

Determining the best instrumentation for your patients and practice is essential for long-term success and profitability. In my practice, I have taken a deliberative approach in which I balance my patient’s needs with the potential return on investment for each piece of equipment I purchase.
My two-OD practice in Silicon Valley, Calif., has been on a quest of updating instrumentation, and taking patient care into the 21st century, since I purchased this 40-year-old practice.
Our practice has a support staff of four, conducts approximately 3,500 annual exams, and brings in $1,300,000 annually. With an updated arsenal of equipment, and doctors who are passionate about patient care, we seek to provide the best care possible to the most amount of patients, while also increasing profitability.
When I first started at Los Altos Optometric Group, I made it imperative that we obtain an OCT in order to decrease the amount of referrals out we needed to make, and to increase the amount of referrals in. Additionally, instrumentation, such as our anterior segment camera and fundus camera, were rarely used, so I implemented guidelines for use of this instrumentation whenever necessary to help us provide more complete care and boost profitably. I saw the use of the ptosis and plaquenil screener on our visual field, and began marketing that to other MDs and ODs in the area for referrals, which has helped us as well.
Rather than thinking only about the money, I think about two aspects of instrumentation:
1) The need for the machine (not the want, because as optometrists we want every new toy possible).
2) How an instrument will help with patient care and set us apart as a practice at the forefront of technology and excellence.
If I can reconcile both of these, then I know that I can provide a vital and pertinent service to patients with the instrument, and in turn, the money will follow.
Assess Current Instrumentation
Here is a run-down of the instruments I have so far added to my practice, including the cost and how I acquired each, and the return on investment.
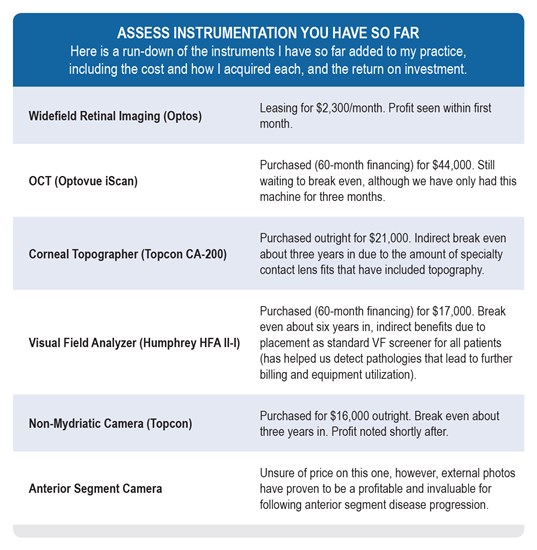
Assess Usefulness of Each Instrument to Patients
Optomap: Used on 90 percent of patients, this is definitely a huge revenue generator in our practice. This is considered elective/screening, so no billing codes, however it can sometimes serve as an appropriate fundus photographer when our non-mydriatic camera cannot capture a good image (ex: a peripheral retinal tear).
OCT: Used on about 10 percent of patients. We use our OCT to get a better look at a variety of retinal pathologies, for glaucoma work-ups, for certain corneal pathologies, and for fitting scleral contact lenses. We have also implemented the iWellness exam (a macular cube screener) as an add-on to the Optomap–a small selection of patients opt for this. Useful billing codes are: 92132 for anterior segment, 92133 for optic nerve, and 92134 for retina. It is always useful to remember that other pathologies besides the usual suspects (ex: glaucoma and macular drusen) can be eligible for OCT. Conditions such as ERM, ONH drusen, suspected breaks/tears/detachments, are just a few others that can utilize an OCT to aid in diagnosis and billing.
Corneal Topographer: Used on about 5-8 percent of patients, the topographer is mainly used for keratoconus cases and CRT fits. Since most of our topography patients are specialty CL patients, the topographer fee is lumped into an all-inclusive fit fee. We generally do not specifically bill for the topography, however the 92025 code has been utilized in certain situations if our medical biller deems it as a better possibility of reimbursement.
Visual Field Analyzer: We use the C40 screener on 100 percent of our patients as part of their comprehensive eye examination. This is vital for detection of underlying pathologies that could easily be missed with Confrontation VFs and allow the patient to perceive their examination as more advance and comprehensive. For specific billing purposes, we use the VF a lot for glaucoma (24-2), plaquenil use (10-2), ptosis screening, and visual field disturbances detected with C40. The 92081-92083 codes serve for billing purposes, which generate a fair amount of revenue, but more importantly, the VF serves as an important aspect of patient care in a variety of pathologies.
Non-Mydriatic Camera: Used on about 10 percent of patients. Our main use for our fundus camera is for glaucoma work-up and following retinal pathology in the posterior pole. I often feel that fundus photography is an under-utilized, yet extremely, valuable instrument. Pathologies such as macular drusen or chorioretinal nevus are just a few of many conditions where fundus photography can be utilized and billed when working with medical insurance. The 92250 code serves for this test.
Anterior Segment Camera: Used on about 10 percent of patients. Another under-utilized test, following a variety of conditions such as blepharitis can benefit from external photography. Additionally, many Medicare patients will have a condition that can be followed with external photography. Be sure to fully utilize this useful tool. The 92285 code serves for this test.
*Note: 92250 and 92285 codes are inherently bilateral.
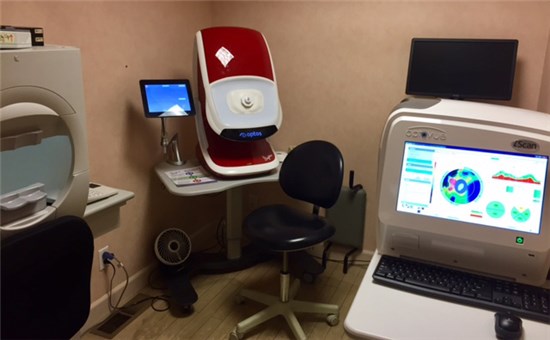
Instrumentation in Dr. Neufeld’s office. Dr. Neufeld says investing in the right instrumentation enables you to provide full-scope medical eyecare, and creates a practice-differentiator, setting you apart from many of your competitors.
Determine Whether an Instrument Requiring Out-of-Pocket Patient Payment Makes Sense
Use of our Optomap requires out-of-pocket payment, but we have found it to still be a worthwhile investment. When deciding whether to add an instrument that requires the patient to pay out-of-pocket, make a checklist of likely advantages. Here is our checklist of advantages offered by the Optomap:
HIGH-QUALITY IMAGE. It allows us to save a high-quality image in the patients file, make notes directly on the image and provides a reference photo for future examinations.
PATIENT ENGAGEMENT. It allows the patient to become engaged, informed and excited about their retinal health. During my review of Optomap images, I always get the patient involved by looking at the image and explaining what the different structures in the retina are, what they do, and how any noted pathology can affect these structures. In fact, this educational journey “through the eye” often serves as a great marketing tool.
REFERRALS. It becomes a word-of-mouth topic for generating referrals. I have had many patients who do one of two things after viewing Optomap images: A) They request the images and show them to friends and family (we even had a couple patients turn the images into works of art and display them at a local community art show) B) They perceive the benefit of the test and “require” less willing family members or friends to have the test done, thus boosting the capture rate.
FULL-SCOPE CARE. It lets us perform a full retinal examination on a patient who may have never had one via dilation. Many patients have told me that if it were not for the Optomap, they would have continued to refuse dilation year after year. In one particular 15-year-old patient, who did not have DFE done for over five years (due to aversion of eye drops), I found a large asymptomatic rhegmatogenous retinal detachment via Optomap (and confirmed via DFE). Two days later, he was having a scleral buckle at our local retinal specialist!
EFFICIENCY. It helps keep us efficient and allows us to see more patients in a day. Plain and simple, dilating every patient creates a considerable amount of time and work. It also puts a strain on patients. They become irate from waiting and the associated side effects.
PRACTICE-DIFFERENTIATOR. It sets us apart as being technologically advanced. While it may just be a part of the variety of machines that convey an innovative and advanced environment of excellence, it plays into a patient’s perception. Many patients comment on the advanced nature of the machine and how it makes them feel more confident in our office and our ECPs. We will have patients who come in and make sure that “we do not forget to the do the Optomap,” while others suggest that we should be charging more for the technology!
Ultimately, the success of any test or procedure that is an out-of-pocket expense revolves around marketing the value of the test to your patient’s health, and to a lesser extent, playing to factors of convenience and your technologically inclined expertise.
Related ROB Articles
Be Smart in Financing Instrument Purchases
Add Full Instrumentation to Succeed with Medical Optometry
Maximize Instrument Use to Enhance Care & Profitability
Related ROB Video
Buy Smart: Upgrade Economically with Used Equipment
Aaron Neufeld, OD, is the owner of Los Altos Optometric Group in Los Altos, Calif. To contact: aneufeldod@gmail.com



























